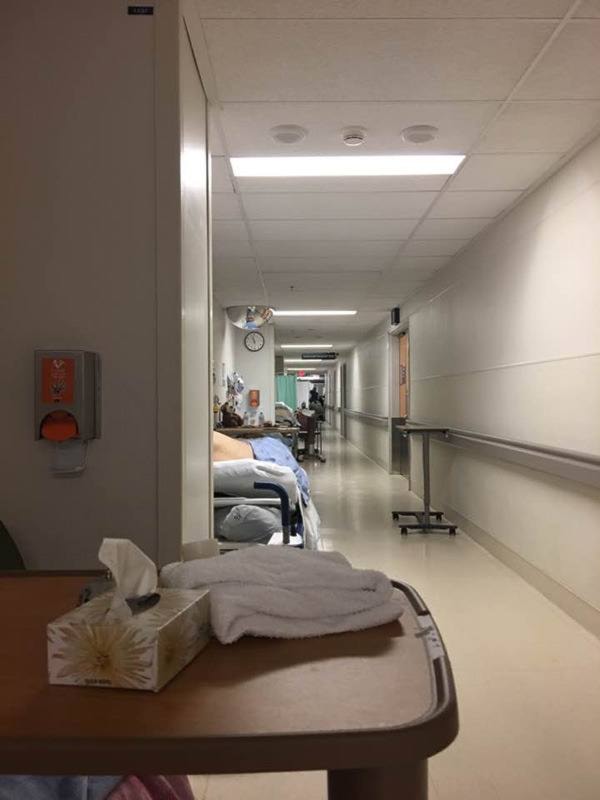
SURREY — The BC Nurses' Union and patients are speaking out about beds lining the hallways of Surrey’s emergency department.
It’s not a rare occurrence – it's actually the norm, according to the union.
Longtime Surrey resident Karen Reid-Sidhu said she was put in a hallway bed last month after being admitted for internal bleeding. During her visit, she counted 35 people in such beds.
“I rarely get sick and this was such a shock to see,” she told the Now.
“The nurses kept apologizing. How sad is that?”
Reid-Sidhu said she was admitted on a Saturday night and after a procedure on a Monday morning was sent back to a hallway bed, before being sent home that night.
“I was so cold in the hallways,” she recalled, explaining she was near the ambulance entrance. “And the air conditioning was blowing over my head. They had to give me medicine for a migraine.”
 She resorted to setting up a makeshift bed with blankets and a pillow on a couch in the family room just to get warm (pictured).
She resorted to setting up a makeshift bed with blankets and a pillow on a couch in the family room just to get warm (pictured).
“I asked my husband to bring me my down slippers because I was freezing,” she recalled.
Reid-Sidhu described the available washroom facilities as “disgusting.”
“There was urine on the floor,” she said, adding she had to repeatedly asked for it to be cleaned.
“It has nothing to do with professional medical providers in there, the nurses and doctors were outstanding. It has nothing to do with them and everything to do with the fact that the system is broken. It needs to be evaluated and fixed. It’s only going to get worse.
“The next time I get sick, I won’t be going to Surrey Memorial Hospital,” she said. “I’m getting my husband to drive me into Coastal Health.”
Meanwhile, Meredith McClurg sent a video to Global News this week after her husband was also stuck in a hallway bed.
BC Nurses’ Union Vice-President Christine Sorensen said the overcapacity hallway issue at Surrey Memorial Hospital has been a problem since the opening of the new tower, and even before that.
“This is not something new. This is something that’s been ongoing,” Sorensen told the Now. “I think people believe or have reported that this only occurs infrequently during specific situations such as a flu outbreak. Unfortunately, that’s not what the nurses are experiencing. It’s a regular situation on most days throughout the hospital.”
She said last Monday at 7 a.m., union stewards counted 24 patients in hallway beds in the emergency department.
“People think this may only occur on a Friday or Saturday night, related to activities on the weekend. Unfortunately that’s not necessarily true,” said Sorensen. “On a Monday morning, to see 24 patients in the hallways tells me that the hospital is full. Patients need to be admitted to other units to get the care that they need and they’re not able to do that. They have probably been there over the weekend.”
While the number of patients in hallways in a given day varies, Sorensen added, “there are never days where there are no patients in the hallways.”
“We certainly had large expansion through a new emergency department there but certainly, we still continue to see patients who are seen in emergency, then admitted, placed in hallways, even emergency department hallways, while waiting for bed placement in another department,” she said, adding it’s not unusual for patients to wait several days there.
But it goes further than hallways, according to Sorensen.
Patients are “sometimes in shower rooms, sometimes in sun rooms, sometimes in lounges," she said.
There are a plethora of issues that come with hallway beds, she explained. Lack of patient privacy is a concern of the union, as is limited access to bathrooms and sinks.
“My understanding is that Fraser Health has gone so far as to install oxygen in hallways, so it’s now looking like these are permanent hallway beds,” she added.
“All of this compromises the patient’s ability to heal and get better. Hallways are not the appropriate setting to allow for safe patient care.”
The solution, according to Sorensen, lies in appropriately staffing community facilities, like senior and mental health care homes.
“I think there has been an effort by Fraser Health to reduce the number of inpatient hospital beds. We do want patients cared for at home, in their long-term care facilities, we support that, but those patients and those clients in the community need the appropriate nursing care who can provide the care in those places and keep them there. But there are just not enough nurses in those facilities.”
Because of understaffing, Sorensen said “patients become ill and seek help in an acute care facility so they come into the emergency department.”
This news comes after Fraser Health Authority closed 80 acute care hospital beds in the valley in February 2016 as part of a plan to expand community and home-based programs.
See more: Fraser Health cutting 80 acute care hospital beds
Fraser Health spokeswoman Tasleem Juma said the health authority is aware of the overcrowding issues and is making efforts to increase community support and capacity to alleviate the crowding.
She said those efforts include an additional 860 hours per day over last year for home health supports, which involves care aids going into homes to help people stay there, as opposed to deteriorating and ending up in hospital.
“And we’ve increased residential care beds by 400,” said Juma, of which a portion are in Surrey. “We also have quick response case managers in the emergency department… and they redirect patients who don’t need acute care back to community supports.
Juma said Surrey’s emergency department sees an average of 55 more patients a day than it did two years ago - anywhere from 450 to 500 a day.
“Our emergency department’s don’t turn people away so congestion and patient volumes is something that’s an issue across the country and our volumes have been increasing across the region. We know that at Surrey in particular, it’s been quite significant.”
Total number of visits to Surrey Memorial Hospital’s emergency department rose from 121,691 in 2014/15 to 141,884 in 2016/17.
“They see an incredible number of people come through the door,” she stated.
When it comes to the oxygen installed in hallways, Juma said that was part of the hospital’s recent expansion and was designed to handle a "mass casualty" scenario.
As for the union’s assertion that patients are being sent to places like shower rooms, Juma said she couldn’t comment without more details of specific instances, but added “recently, I’m not aware of any of those situations happening.”